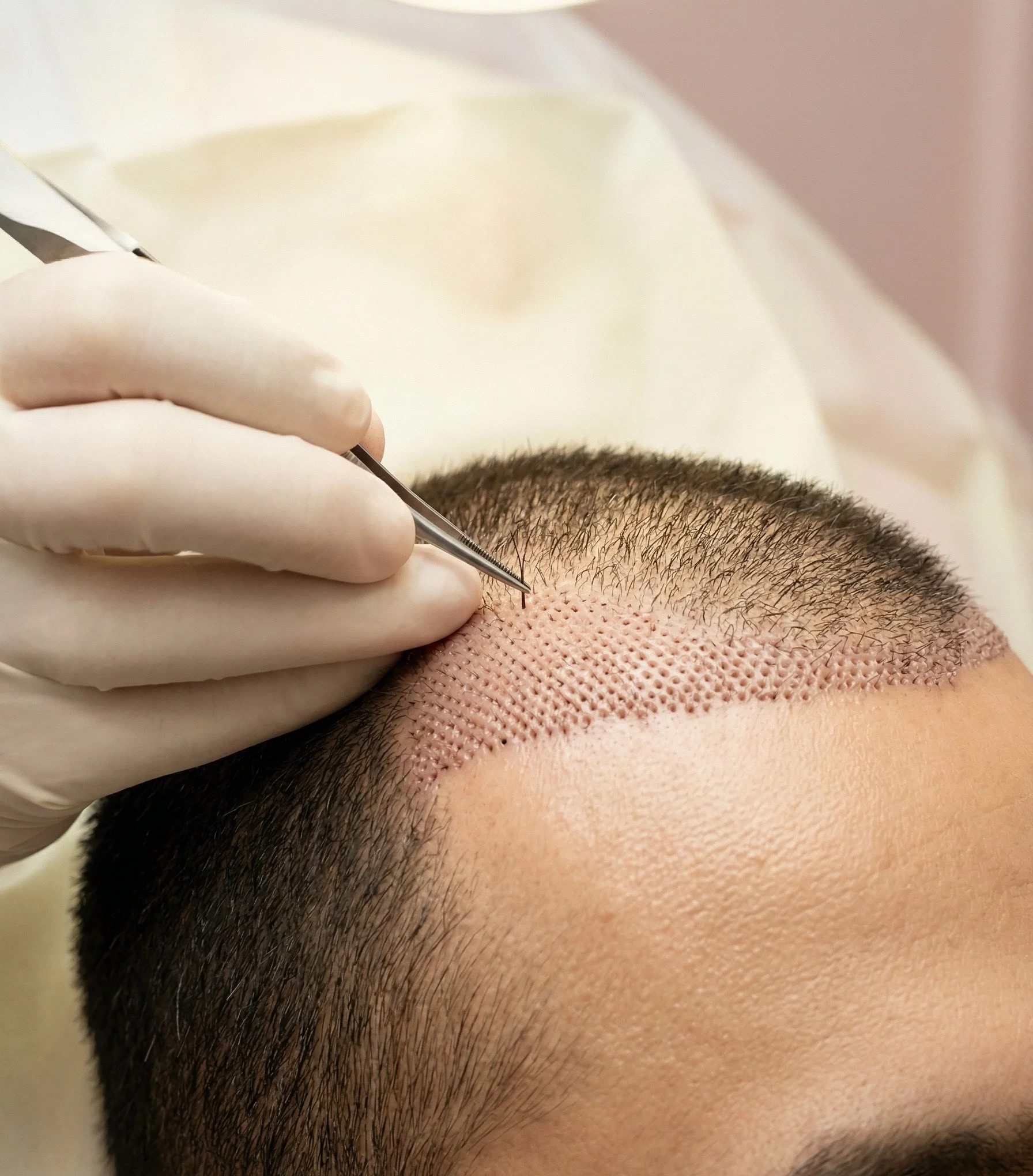
A hair transplant is a surgical procedure with a predictable recovery arc — but one that many patients aren't fully prepared for, particularly the phase called "shock loss." Understanding what is normal at each stage will prevent unnecessary anxiety and help you take care of your scalp correctly during the healing process.
The Day of the Procedure
FUE (Follicular Unit Extraction) involves extracting individual hair follicles from the donor area (typically the back and sides of the scalp) and implanting them in the recipient (thinning) area.
The procedure is performed under local anaesthesia and typically takes 6–8 hours depending on the number of grafts. Most patients are comfortable throughout, though there can be a sensation of pressure or mild discomfort as the anaesthesia is administered.
You will leave the clinic with the transplanted grafts visible as small dots across the recipient area, and the donor area will have pinpoint scabs from the extraction sites.
Days 1–3: Swelling and Tenderness
Some swelling around the forehead and sometimes around the eyes is normal and peaks around day 2–3. This is not a sign of infection — it is simply the result of the fluids used during the procedure moving downward with gravity.
The grafts at this stage are fragile. You should:
- Sleep with your head elevated (at a 45-degree angle) to minimise swelling
- Avoid touching, scratching, or pressing on the recipient area
- Follow the prescribed antibiotic and anti-inflammatory medication schedule
Days 4–7: Crust Formation
Small crusts will form around each transplanted graft. These are part of the normal healing process. Do not pick at them.
Your doctor will instruct you on when and how to begin gentle washing — typically from day 4 or 5 onward, using a specific technique to keep the area clean without dislodging grafts. The donor area heals faster and usually looks largely normal by the end of the first week.
Avoid direct sun exposure to the scalp during this period.
Weeks 2–3: Shock Loss Begins
This is the stage that surprises — and worries — many patients.
Around 2–3 weeks post-transplant, the transplanted hairs begin to shed. This is normal and expected. It is called telogen effluvium or shock loss, and it happens because the trauma of transplantation temporarily shifts the follicles into a resting phase.
What you see shedding is the hair shaft — the follicle (the living root) remains in the scalp. New growth will come from the same follicles.
Some patients also notice temporary thinning in the native (non-transplanted) hair near the procedure area during this period, for the same reason.
This phase can look disheartening. It is one of the most important things to be prepared for mentally before undergoing the procedure.
Months 1–3: The Dormant Phase
The transplanted follicles are present in the scalp but largely inactive. The recipient area may look sparse. There is very little visible change during this window.
This is also the time when the donor area fully heals and the small circular scars from FUE extraction fade to become imperceptible under hair.
Patience is required here. This phase is not a sign that the transplant has failed.
Months 3–4: First Signs of Growth
Around the 3-month mark, fine, thin new hairs begin to emerge from the transplanted follicles. These hairs are initially soft and may be slightly lighter in colour — this is normal.
Growth is typically uneven at this stage. Some areas of the recipient zone may show new hair while others appear to lag. This usually evens out over subsequent months.
Months 6–9: Meaningful Density
By 6 months, the majority of transplanted hairs are growing. The result looks recognisably better than before the procedure, and most patients feel comfortable without concealment.
The hairs at this stage are also maturing — becoming coarser and more pigmented as the follicle fully re-establishes itself.
Month 12: Final Assessment
The full result of a hair transplant is assessed at 12 months. By this point:
- Transplanted hairs are at their natural thickness and texture
- The hairline or density in the recipient area reflects the final surgical outcome
- Any decision about a second session (if more coverage is desired) can be made with full information
Supporting the Result
Several factors support optimal graft survival and growth:
GFC or PRP therapy: Scalp injections can be performed starting around 1 month post-transplant and repeated every 4–6 weeks to support graft survival and improve native hair density.
Medications: If androgenetic alopecia (pattern hair loss) is ongoing, medical treatment to stabilise the loss in the non-transplanted areas is important. A transplant addresses existing baldness; it does not prevent future loss in untreated areas.
Scalp care: Avoid aggressive chemical treatments, excessive heat, and tight hairstyles during the recovery period.
What a Realistic Result Looks Like
A well-performed FUE transplant in a suitable candidate produces a significant, natural-looking improvement in hairline restoration or density. The result is permanent in the transplanted area — these follicles are harvested from regions of the scalp that are genetically resistant to DHT-induced miniaturisation.
What it cannot do: replace more hair than was harvested. Donor supply is finite, and planning the placement of grafts carefully — prioritising natural-looking hairline design and long-term density — is as important as the surgical technique itself.
If you are considering a transplant and are unsure whether you are a suitable candidate, a trichoscopy assessment (scalp examination under magnification) at consultation will provide a clear picture of your donor density and recipient area requirements.